Laparoscopic Gallbladder Surgery
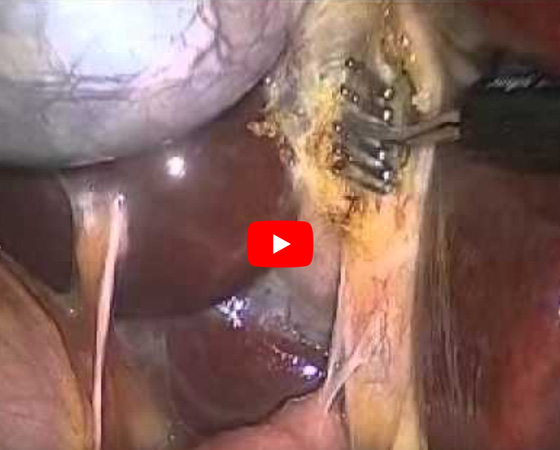
Laparoscopic Cholecystectomy Operative video
What are gallstones?
The gallbladder is a small, pear-shaped pouch in the right upper abdomen under your liver. Bile is made in the liver and then stored in the gallbladder until the body needs it - it helps the body to digest fat. Gallstones form when liquid bile hardens into pebbles, usually because it contains too much cholesterol, bile salts, or bilirubin.
What symptoms may I suffer from if I have gallstones?
Gallstones can cause intermittent upper abdominal pain, bloating, heartburn or pain in the right shoulder or back, usually after a rich meal. Sometimes gallstones can cause symptoms by causing inflammation of the gallbladder (cholecystitis) or pancreas (pancreatitis) and present with persistent pain, nausea, vomiting, fever or jaundice.
How are gallstones diagnosed?
Gallstones are usually diagnosed with ultrasound scans. Sometimes, these can be detected with other investigations like CT scan, MRI scan etc. Abnormal blood tests in the presence of appropriate symptoms may suggest the presence of gallstones.
What treatments are available for gallstones?
Gallstones can be treated conservatively in a small proportion of patients by restricting fat in the diet and with painkillers. Unfortunately, 80 to 100% patients with gallstone have recurrent or progressive symptoms or complications over ten years and will require removal of the gallbladder (cholecystectomy). The risks of conservative management include recurrent symptoms and the development of complications like cholecystitis, cholangitis, obstructive jaundice, biliary fistulae, gallstone ileus, acute pancreatitis, empyema of gall bladder and mucocele. There is also a 5% risk of developing gall bladder cancer over 25 years. These risks are there even if you stick to a low fat diet for the rest of your life.
What happens at the first appointment?
Your surgeon will initially take a history, examine you and perform appropriate tests to identify the cause of your symptoms. He will also ensure that you are fit to undergo any procedure / surgery and an anaesthetic. He may also suggest initial trial of medical treatment for your symptoms.
What happens at the subsequent appointments?
He will check that all necessary information and reports are available and have been evaluated. He will discuss the results and reports of various investigations. He will assess your response and satisfaction with the trial of medical treatment for your symptoms. He will discuss with you the various options available to treat your symptoms. If you want to undergo gallbladder surgery then he will agree with you a date for the procedure.
Admission for surgery
You must not eat any food from 6 hours before the operation. You are allowed to drink clear fluids, including tea and coffee without milk up to 3 hours before the operation. A nurse will admit you on the day of surgery. The surgeon and the anaesthetist will see you prior to your operation. They will confirm that you are willing to undergo surgery, all preparations are complete and it is safe to proceed with your operation. They will confirm that an appropriate facility is available for you to recover after surgery.
What happens during surgery?
The operation is performed under general anaesthetic and a small ‘telescope’ (laparoscope) is passed into your abdomen above the navel. Your abdomen is filled with carbon dioxide gas, to help see everything properly. Further 2-3 small cuts will be made in your abdomen to insert instruments to help with the operation. The surgeon will disconnect the gallbladder from the plumbing of the liver (bile duct) and then remove the organ.
What happens in hospital after surgery?
You will be sent to the Ward after the procedure. You will be looked after by a nurse and offered appropriate pain-killers. You will be offered light food and drink. Usually the procedure is performed as a day case and you will be able to return home on the same day, when it is safe to do so. You will need to have a responsible and capable adult to take you home and to look after you for the first 24 hours. You should not operate machinery during this period. You will have a few small wound dressings which you can remove yourself after one week or a nurse / the surgeon can remove these at a subsequent visit.
You may be kept in hospital for a longer period if you have additional medical problems or if you live alone.
Support available during early recuperation period after surgery
It is advisable to avoid strenuous physical activity for the first 2 weeks to allow proper healing of the wounds. It is usual for you to experience some initial difficulty in swallowing and pain in the wounds - you may also experience minor discomfort in the shoulder. Most patients recover fully within 1-2 months. You will be given a number to ring for advice in case of difficulty.
Further follow up after surgery
You will be given an appointment to see the surgeon again - he will ensure that you are recovering as expected.
Will further surgery be needed?
This is usually not necessary, though rarely surgery may be required if you develop complications.
Gallstones can be treated conservatively in a small proportion of patients. Unfortunately, 80 to 100% patients with gallstone have symptoms and complications over ten years leading to a cholecystectomy. The risks of conservative management include dietary restriction, cholecystitis, cholangitis, obstructive jaundice, biliary fistulae, gallstone ileus, acute pancreatitis, empyema gall bladder, mucocele and recurrent symptoms. There is also a 5% risk of developing gall bladder cancer over 25 years. These risks are there even if she sticks to a low fat diet for the rest of her life.
Since she had previous pain and jaundice, therefore it is recommended that she undergo a laparoscopic cholecystectomy. This involves making 3-4 small cuts in her abdominal wall and removing her gallbladder with its contents under a general anaesthetic. There is a 5% risk of requiring an open surgery and the risks include infection, bleeding, injury to surrounding structures including bile duct necessitating corrective procedures (0.02%), thrombo-embolism (clots in leg veins), bile leak, retained stones, port site or incisional hernia and rarely chronic pain from biliary dysfunction in a small number of patients. There is also a 10% risk of slight change in bowels towards looser motions. The risk of mortality from this type of surgery is very small.
I have put her name on the waiting list to undergo a laparoscopic cholecystectomy with an on-table cholangiogram (dye test), to avoid unnecessary delay. If she is agreeable, then she does not need to take any further action. I will complete the consenting process and discuss the risks and benefits of operation on the day of her admission. Assuming that she is fit, then she will undergo a day case operation and will be discharged home on the same day. There is a 1-4 week (av. 2 week) recuperation period depending on the nature of her work, assuming that the operation is completed with keyhole surgery. In the event of converting to an open procedure, she may require 6-12 weeks. In the event of converting to an open procedure, she may require 6-12 weeks of recuperation.

|